ATD Blog
Healthcare Simulation: Team Training Strategies for Quality Patient Care
Fri Jun 12 2020
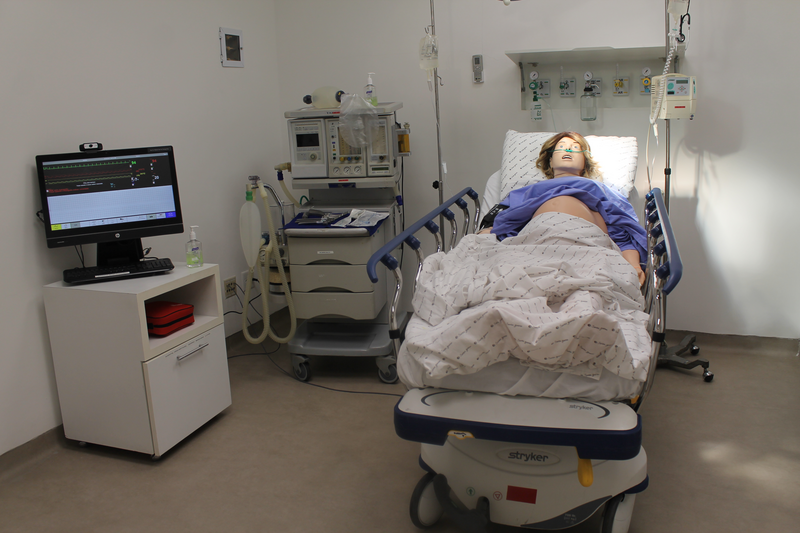
What do these have in common?
computerized mannequin (with life-like monitors) that talk, breathe, and react to participant actions and inactions
trained medical actors (called standardized patients or SPs) who portray patients, clinicians, family members, and others in the healthcare environment
devices that mimic the feel of doing surgery and other procedures (called haptics)
virtual reality applications that immerse participants in a highly emotional clinical scenario
life-like models of body parts (called procedural task trainers) that can be used to practice specific skills, such as starting intravenous lines or placing breathing tubes
These are examples of how healthcare simulation modalities are transforming the learning experience for healthcare providers, patients, and families. The widespread adoption of simulation science and simulation-based training within the preprofessional schools and healthcare arenas have transformed how healthcare providers are currently being introduced to the concepts of team training, improved communication, and procedural skills mastery for patient-centered care.
Healthcare simulation is often associated with the broad use of technology. In fact, the term high-fidelity simulation has been used to refer to the use of advanced computerized mannequins that can interface with the learners in a meaningful, real-time fashion. Although technological advancements have helped create a level of clinical realism that is far more immersive than in the past, simulation science is more than the equipment or technology. In fact, simulation is a teaching science that integrates experiential learning with facilitated debriefing. The goal of the debriefing period is to enhance each participant’s engagement with the topic and to facilitate their ability to transfer the knowledge, skills, and attitudes experienced in the simulation session to the actual work environment.
In the clinical settings, including hospitals and outpatient clinics, simulation educators often train nurses, physicians, and other healthcare members of the interprofessional team to handle emergency response situations. Examples of such training include respiratory arrest, cardiac arrest, and other catastrophes such as anaphylaxis, heart attacks, and strokes. Using an advanced computerized mannequin to play the role of the patient along with a well-trained standardized patient (SP) to portray a distraught family member, the level of realism and immersive experience for the learner is vastly enhanced.
For the simulation exercise, the interprofessional emergency response team (“code team”) gathers at the scene and engages in a resuscitative effort on the mannequin, including performing cardiopulmonary resuscitation (CPR), defibrillating or shocking the mannequin if indicated, giving medications, and so forth. In addition to these clinical skills, an important learning objective of the simulation can also be to practice effective teamwork and communication skills, such as demonstrating closed-loop communication to ensure tasks are delegated and completed and providing mutual support to ensure that team members are monitoring each other and providing help as necessary.
When the training is performed in the actual clinical environment, the simulation is referred to as in situ (in the original place). This type of training allows simulation educators to meet the educational needs of healthcare professionals at their place of practice. Additionally, it allows for the identification of latent threats that hinder optimal resuscitation efforts, including faulty emergency alerting and communication systems, lack of appropriately functioning life-saving equipment, and other systems-related issues. Much of these best practice training measures would not be possible without the advances made in simulation science.
In addition to identifying latent threats, simulation has also been successful in bringing together healthcare professionals who, in the past, were more likely to train in silos. Unlike the traditional training environment where nurses train with other nurses and physicians train with other physicians in silos, the simulation learning environment promotes interprofessional team training by placing diverse clinical disciplines in the realistic patient care environment to provide optimal care for the patient. In fact, interprofessional teamwork and interprofessional communication are now considered two of the core competencies that health professions students must possess upon graduation. The objective is to prepare our graduates to optimally perform in the complex health care environment.
The ultimate goal for all healthcare professionals regardless of educational background or experience is to be focused on providing quality patient care. Simulation and facilitated debriefing have been shown to increase participant engagement and provide participants with opportunities to practice skills with team members, reflect on what went well and what could be done differently in the future, and transfer that learning to the workplace environment.
